Rachana Yendala1, Nauman Shahid1, Ahmed Alnemari4, Robert Mrak2, Mark Buehler3, Daniel Gaudin4* and Muhammad Hameed5
1Department of Medicine, The University of Toledo Medical Center,3000 Arlington Avenue, MS #1088, Toledo, OH 43614, USA
2Department of Pathology, The University of Toledo Medical Center,3000 Arlington Avenue, MS #1088, Toledo, OH 43614, USA
3Department of Radiology, The University of Toledo Medical Center,3000 Arlington Avenue, MS #1088, Toledo, OH 43614, USA
4Department of Surgery/Division of Neurosurgery, The University of Toledo Medical Center,3000 Arlington Avenue, MS #1088, Toledo, OH 43614, USA
5West Michigan Cancer Center,200 N. Park Street Kalamazoo, MI 49007
*Corresponding Author:
Daniel Gaudin, MD, PhD, FACS
The University of Toledo Medical Center
3000 Arlington Avenue, MS #1088
Toledo, OH 43614, USA
Tel: (419) 383-3547
Fax: (419) 383-6570
E-mail: daniel.gaudin@utoledo.edu
Received: February 04, 2016; Accepted: February 09, 2016; Published: February 17, 2016
Keywords
Intradural extramedullary ependymoma; Schwannoma; Non-myxopapillary
Abbreviations
IDEM: Intradural Extramedullary; IDIM: Intradural Intramedullary; L: Lumbar; MRI: Magnetic Resonance Imaging; WHO: World Health Organization
Background
Primary spinal cord tumors account for 2%-4% of all primary tumors of the central nervous system [1]. These are anatomically classified into extradural (55%) and intradural (45%) lesions, and further classified into extramedullary (5%) and intramedullary (40%) within the intradural compartment; intradural extramedullary (IDEM) and intramedullary (IDIM) respectively [2]. Meningiomas and nerve sheath tumors predominately constitute IDEMs. About 65% of the latter are schwannomas, which usually arise from the Schwann cells of dorsal nerve roots in the 4th to 6th decade of life [3]. Although a majority are sporadic, 2% of spinal schwannomas occur with neurofibromatosis (NF2) and schwannomatosis [4]. These are commonly multiple and are associated with other coexisting spinal tumors, such as meningiomas and occasionally spinal ependymomas.
Ependymomas, first described by Bailey in 1924, are the most common intramedullary spinal glial tumors in adults; developing from ependymal cells in the ventricle, choroid plexus, central canal of the spinal cord and the filum terminale. Histologically and pathologically, these are classified into cellular (WHO grade II and III) and myxopapillary (WHO grade I). They are mostly benign (low grades I and II), but malignant (WHO grade III–anaplastic) subtypes also occur. The more common cellular or classic variant typically arises in the cervical and thoracic cord while myxopapillary variant arises exclusively at the conus medullaris [5].
Ependymomas are exceedingly rare in the IDEM location and very few cases have been reported in literature since the first case in 1951 by Cooper et al. [2,3]. These tumors tend to occur in the 4th to 5th decade of life and may have a female predominance [2,6]. These are low grade tumors, commonly described in the thoracic and cervical spine. However, malignant transformation including cerebrospinal fluid dissemination and recurrence have been reported [7]. On Magnetic Resonance Imaging (MRI), ependymomas typically appear as a focal enlargement of the spinal cord (intramedullary) that is hypertense on T2W images and hypo- or iso-intense on T1W with heterogeneous contrast enhancement (may have cystic component) [8]. Schwannomas usually appear as solid tumors in the dorsal nerve root region with hyper-intense T2W image features and intense contrast enhancement of the iso-intense T1W images [8]. When presenting together at one location, however, as described in our case, differentiating these tumors can be challenging and the need for early identification is paramount as outcomes differ. We report an IDEM ependymoma synchronously presenting with a spinal schwannoma in a benign setting.
Case Presentation
A 43-year-old female presented to the authors’ institution with chronic nerve dysfunction involving progressive, bilateral leg paresis, radiculopathy and intermittent urinary sphincter disturbances over a span of 7-8 years. Examination showed lumbar (L) spine tenderness, limited range of movements, gait ataxia, decreased muscle strength in lower extremities, hypoesthesia with abnormal vibration and touch sensation. Imaging with MRI L-spine revealed severe L3-L4 canal stenosis with 2 contrast-enhancing IDEM lesions near the inferior conus medullaris, at L2-3 and L4-5 vertebral spaces measuring 8 mm and 5 mm respectively (Figure 1A and 1B), suspicious for drop metastatic lesions versus nerve sheath tumors like schwannoma or meningioma.
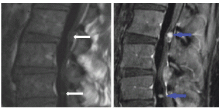
Figure 1: T1 MRI Images: a. MRI w/o contrast - illustration of IDEM tumors at L2-L3 and L4-L5; b. MRI with contact.
Subsequent metastatic work up including CSF analysis showed no leptomeningeal involvement. Owing to mild deficits and multiple lesions, a decompression surgery was performed (laminectomy L2-L5). The larger L2-3 mass was completely resected with microdissection. Preliminarily, frozen section showed a spindled appearance suggestive of a schwannoma. Further intraoperative exploration could not identify the smaller L4-5 mass as noted radiographically and this was left behind. However, permanent histological sections later revealed round to oval cells with minimal atypia and perivascular psuedorosette formation (Figure 2A). By immunohistochemistry, the tumor cells were diffusely positive for CD99 and GFAP and showed patchy positivity for S-100, supporting the diagnosis of ependymoma. Ki-67 immunohistochemistry showed a low proliferative index (<1%) consistent with a WHO Grade II lesion. Repeat imaging for metastases was unremarkable while the L4 IDEM lesion remained stable. Clinically, only a mild improvement in symptoms was noted. The patient was now believed to have a multifocal IDEM ependymoma and repeat surgery was performed to remove the second tumor. Intraoperatively, the mass was localized encasing the L5 nerve root completely and only 50-60% of the mass was safely resected. The final pathology showed an intradural schwannoma predominantly with classic Antoni A pattern (Figure 2B), while the typical features on the two lesions are noted on Electron Microscopy (Figure 3A and 3B). Although significant clinical improvement was noted after the second resection, the patient received radiation therapy for residual symptoms.
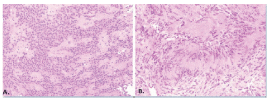
Figure 2: Histological Sections: a. Ependymoma cells with uniform small round nuclei, there are perivascular pseudorosettes; b. Schwannoma spindle cells (Antoni type A area) showing true palisading to produce Verocay bodies (pink zones without nuclei).

Figure 3:Electron Microscopic Images: a. Ependymoma Image (tissue retrieved from paraffin Block) - Two tumor cell nuclei are present in the upper right and lower left. The area between the cell somas does not show interdigitating cell processes or Luse bodies. A few intercellular tight junctions can be discerned. b. Schwannoma Image (tissue retrieved from paraffin block) - Low power electron micrograph showing several spindled cell nuclei, together with many interdigitated cell processes in the areas between the cell somas - UPPER RIGHT INSET: Higher power electron micrograph of the interdigitating cellular processes showing fibrous long spacing collagen (Luse body), typical of a Schwannoma.
Discussion
IDEM tumors include meningiomas and nerve sheath tumors (schwannomas, neurofibromas). Excluding those occurring at the conus medullaris and filum terminale, 20 cases of IDEM ependymomas have been described to date, only two of which involved a multifocal presentation [2,6]. The majority of these involved the thoracic region, in contrast to intramedullary ependymomas, which are predominantly cervical [8-10]. Our case is unique in terms of location and presentation - a lumbar non-myxopapillary IDEM ependymoma coexisting with a sporadic schwannoma, which to the best of our knowledge has never been reported before.
Occurrence of multiple spinal tumors are rare (1%-4%) involving schwannoma, meningioma and, less commonly, spinal ependymoma (in the context of Von Recklinghausen disease [11]. It is often difficult to identify this kind of presentation (central neurofibromatosis group, classified based on neurological manifestations), which show only minimal cutaneous manifestations. Some authors have also described a sporadic, non-inherited variant of neurofibromatosis characterized by multiple spinal tumors, usually with cutaneous neurinomas [12]. Historically, very few cases of schwannoma and medullary ependymomas have been described in the absence of phacomatosis, which could represent a mild form of neurofibromatosis [11,13,14].
The pathogenesis of extramedullary ependymal is not clear. One hypothesis is that IDEM tumors arise from heterotopic ependymal cell nests left in the extramedullary space as the neural tube closes. Another theory suggests that they originate from invaginations of the neuroaxis into the extramedullary space. Both of these theories are supported in the description by Cooper et al. [7]. A hormonal mechanism is also thought to play a role in the development of this rare tumor, as suggested by Duff et al. [15], which would explain the female predominance [15,16], but this was not confirmed by cytogenetic or molecular studies. Additionally, development of schwannomas is well known to be precipitated by micro trauma and irritation which could possibly explain the concomitant occurrence in our patient [14]. This hypothesis of one tumor stimulating another to develop has also been described by some authors in cases of multiple cerebral tumors [17].
The clinical presentation of IDEM ependymal is similar to other, more common extra medullary tumors and depends upon the location of the tumor, with dorsalgia and radicular pain commonly reported [6]. It usually takes a few months to years from the onset of symptoms to reach a diagnosis (probably because of the use of conservative measures to treat the back pain symptoms before using more advanced imaging studies). Contrast enhanced MRI of the spine is the investigative study of choice. IDEM ependymomas appear as well-delineated tumors located within the dural space that enhance homogeneously after administration of contrast material. These findings are often first diagnosed as meningioma or schwannoma [18,19]. There are no specific radiologic features of an IDEM ependymoma, which highlights the role of surgical resection and histopathological identification in definitive diagnosis [20].
Treatment of ependymoma involves primarily maximum safe surgical resection with a probable role of radiation and chemo treatment in the event of malignant transformation or recurrence [21,22]. Schwannomas are often surgically treated when symptomatic (pain or neurological deficit) or in case of complications (bleeding or disfigurement) while some (asymptomatic/low malignancy suspicion) can be followed with observation [23]. In our case, although the IDEM ependymoma was completely resected, the patient was referred for radiation treatment on account of her symptomatic schwannoma. The clinical outcome was mainly determined by the extent of resection and presence of meningeal infiltration rather than by the underlying histology itself [6]. Despite a good outcome initially, cases of recurrence with malignant transformation have been reported [7]. Hence, long-term prognosis remains to be established through careful MRI surveillance.
Conclusion
IDEM ependymomas should be included in the differential of intradural extramedullary tumors. These have the potential to coexist with other closely mimicking tumors, and this should be taken into account in patients with multiple spinal lesions. Owing to the potential for malignant transformation and tumor dissemination, timely surgical resection followed by timely surveillance needs to be considered in the outcome and management.
Acknowledgements
The authors would like to thank Teri Diehl, Department of Surgery/Division of Neurosurgery, The University of Toledo Medical Center, for assisting in the preparation of this paper.
8492
References
- Chamberlain MC, Tredway TL (2011) Adult primary intradural spinal cord tumors: a review. Curr Neurol Neurosci Rep 11: 320-328.
- Guarnieri G, Tecame M2, Izzo R3, Zeccolini F2, Genovese L4, et al. (2014) Multisegmental diffuse intradural extramedullary ependymoma. An extremely rare case. Neuroradiol J 27: 179-185.
- el-Mahdy W, Kane PJ, Powell MP, Crockard HA (1999) Spinal intradural tumours: Part I--Extramedullary. Br J Neurosurg 13: 550-557.
- Murray AJ, Hughes TA, Neal JW, Howard E, Evans DG, et al. (2006) A case of multiple cutaneous schwannomas; schwannomatosis or neurofibromatosis type 2? J Neurol Neurosurg Psychiatry 77: 269-271.
- Louis DN, Ohgaki H, Wiestler OD, Cavenee WK, Burger PC, et al. (2007) The 2007 WHO classification of tumours of the central nervous system. Acta Neuropathol 114: 97-109.
- Iunes EA, Stávale JN, de Cássia Caldas Pessoa R, Ansai R, Onishi FJ, et al. (2011) Multifocal intradural extramedullary ependymoma. Case report. J Neurosurg Spine 14: 65-70.
- Robles SG, Saldaña C, Boto GR, Martinez A, Zamarron AP, et al. (2005) Intradural extramedullary spinal ependymoma: a benign pathology? Spine (Phila Pa 1976) 30: E251-254.
- Abul-Kasim K, Thurnher MM, McKeever P, Sundgren PC (2008) Intradural spinal tumors: current classification and MRI features. Neuroradiology 50: 301-314.
- Yoshii S, Shimizu K, Ido K, Nakamura T (1999) Ependymoma of the spinal cord and the cauda equina region. J Spinal Disord 12: 157-161.
- Bourgouin PM, Lesage J, Fontaine S, Konan A, Roy D, et al. (1998) A pattern approach to the differential diagnosis of intramedullary spinal cord lesions on MR imaging. AJR Am J Roentgenol 170: 1645-1649.
- Nishiura I, Koyama T, Tanaka K, Aii H, Amano S (1989) The occurrence of different types of spinal tumours in one patient. A case report and review of the literature. Neurochirurgia (Stuttg) 32: 52-55.
- Daras M, Koppel BS, Heise CW, Mazzeo MJ, Poon TP, et al. (1993) Multiple spinal intradural schwannomas in the absence of von Recklinghausen's disease. Spine (Phila Pa 1976) 18: 2556-2559.
- Heuschling C, Cardon T, Assaker R, Ruchoux MM, Chastanet P, et al. (1995) Neurilemoma and ependymoma of the spinal cord in the same patient. A case-report. Rev Rhum Engl Ed 62: 401-403.
- Sciolla R, Sicuro L, Regolo P, Pagni CA (1987) Multiple diverse intracranial and intramedullary spinal tumors. Report of a case. J Neurosurg Sci 31: 191-194.
- Duffau H, Gazzaz M, Kujas M, Fohanno D (2000) Primary intradural extramedullary ependymoma: case report and review of the literature. Spine (Phila Pa 1976) 25: 1993-1995.
- Cheng CH, Lee TC, Huang HY, Lui CC (1996) Extramedullary thoracic myxopapillary ependymoma--a case report of a rare tumour. Ann Acad Med Singapore 25: 869-872.
- Arseni C, Constantinescu A, Dănăilă L, Carp N (1975) Multiple cerebral tumours of varying histologic origin. Neurol Psychiatr (Bucur) 13: 111-116.
- Li MH, Holtås S (1991) MR imaging of spinal intramedullary tumors. Acta Radiol 32: 505-513.
- Sun B, Wang C, Wang J, Liu A (2003) MRI features of intramedullary spinal cord ependymomas. J Neuroimaging 13: 346-351.
- Ando K, Imagama S, Ito Z, Hirano K, Tauchi R, et al. (2014) Differentiation of spinal schwannomas and myxopapillary ependymomas: MR imaging and pathologic features. J Spinal Disord Tech 27: 105-110.
- Abdel-Wahab M, Etuk B, Palermo J, Shirato H, Kresl J, et al. (2006) Spinal cord gliomas: A multi-institutional retrospective analysis. Int J Radiat Oncol Biol Phys 64: 1060-1071.
- Lee SH, Chung CK, Kim CH, Yoon SH, Hyun SJ, et al. (2013) Long-term outcomes of surgical resection with or without adjuvant radiation therapy for treatment of spinal ependymoma: a retrospective multicenter study by the Korea Spinal Oncology Research Group. Neuro Oncol.;15: 921-929.
- Tiel R, Kline D (2004) Peripheral nerve tumors: surgical principles, approaches, and techniques. Neurosurg Clin N Am 15: 167-175, vi.








