Ersin Gürkan Dumlu1*, Mehmet Tokaç1, ÃÆÃââââ¬Ã
¾ÃÆââ¬Å¡Ãâðbrahim KÃÆÃââââ¬Ã
¾ÃÆââ¬Å¡ÃâñlÃÆÃââââ¬Ã
¾ÃÆââ¬Å¡Ãâñnç1, Murat Baki YÃÆÃââââ¬Ã
¾ÃÆââ¬Å¡ÃâñldÃÆÃââââ¬Ã
¾ÃÆââ¬Å¡ÃâñrÃÆÃââââ¬Ã
¾ÃÆââ¬Å¡Ãâñm1, Abdussamed YalçÃÆÃââââ¬Ã
¾ÃÆââ¬Å¡Ãâñn2 and Mehmet KÃÆÃââââ¬Ã
¾ÃÆââ¬Å¡ÃâñlÃÆÃââââ¬Ã
¾ÃÆââ¬Å¡Ãâñç2
1Atatürk Training and Research Hospital, Department of General Surgery, Ankara, Turkey
2YÃÆÃââââ¬Ã
¾ÃÆââ¬Å¡ÃâñldÃÆÃââââ¬Ã
¾ÃÆââ¬Å¡ÃâñrÃÆÃââââ¬Ã
¾ÃÆââ¬Å¡Ãâñm BeyazÃÆÃââââ¬Ã
¾ÃÆââ¬Å¡Ãâñt University, Faculty of Medicine, Department of General Surgery, Ankara, Turkey
- *Corresponding Author:
- Ersin Gürkan Dumlu, MD
Atatürk Training and Research Hospital
Department of General Surgery
Ankara, Turkey
Tel: +905324465043
E-mail: gurkandumlu@gmail.com
Keywords
Mastectomy, Prophylactic mastectomy, Breast carcinoma
Introduction
Following prophylactic mastectomy (aka bilateral risk-reducing mastectomy), the incidence of breast carcinoma is presumably not more than 2% [1]. The studies by Pennisi and Capozzi [2] and Woods [3], among several others, reported that a few out of more than 1,000 patients in their studies (prophylactic subcutaneous mastectomy) developed breast cancer after years of follow-up (incidence rate 0.6%). Yet, nipple sparing mastectomy raises some major concerns one of which is that when it is used for prophylaxis, it poses persistent risk of developing breast cancer. Besides, there is lots of controversy in terms of oncological perspective regarding the safety of such procedures [4,5]. It has been reported that prophylactic bilateral mastectomy decreases risk of breast cancer by more than 80% [6]. Vulnerability to cancer-specific worry is often found with women who have consistently estimated too highly about their risk of breast cancer [7]. This situation might push such women to take unusual measures against breast cancer including having a prophylactic bilateral mastectomy. Breast cancer risk assessment is a method to discover the quantity of lifetime probability of a certain woman’s developing breast cancer. For the time being, risk assessment relies on epidemiologic observations which are derived from defined study populations rather than for individuals.
We report the case of a 46 year-old female who indicated ductal carcinoma following bilateral prophylactic mastectomy.
Case Report
The 46 year-old premenopausal female patient was admitted to our cliniccomplaining about the mass that was felt on her left breast. Since her mother had died due to breast cancer, she had volunteered to go through bilateral prophylactic mastectomy 5 years ago, and she had been given concurrent bilateral breast implant. The patient who had her annual follow-up, physical examination and ultrasound imaging noticed a mass in lower quadrant of her left breast in the last month. During the physical examination, a mass of approximately 1.5 cm was found in lower outer quadrant of her left breast in the region fitting to the edge of the implant. The ultrasonography showed an irregular contour solid lesion indicating microlobulation with dimensions of 1.3 x 1.5 cm in the lower outer quadrant of the left breast lateral to palpation localisation. MR imaging was conducted on the patient. The image found in USG was also confirmed by MR (Figure 1). Moreover, due to the fact that the condition created major concerns for malignity in reference to contrasting pattern of the mass, it was decided to carry out a biopsy. As the result of pathology of excisional biopsy indicated invasive ductal ca, it was decided to carry out extended excisional and axillary dissection on the patient. An incision of 4 cm was done on the left lower quadrant, and the suspected area was removed up to the surface of the implant. Frozen section was performed, and the surgical margins were found to be negative. An incision about 5 cm long was done on axillary, and axillary lymph node was dissected. The patient did not have any problem during postoperative period. She was discharged and referred to oncology department. The pathologic examination is resulted as invasive ductal carcinoma and reactive lymph nodes.
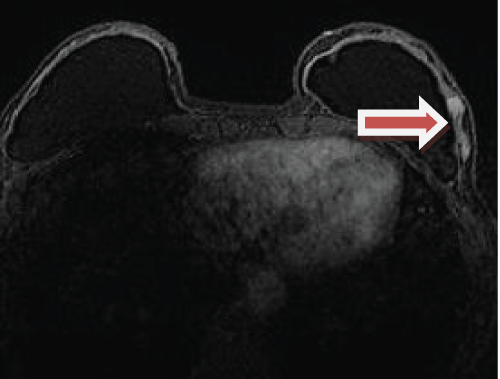
Figure 1: MRI scan of the lesion.
Discussion
As a means of reducing breast cancer risk, surgery is an option for women who has not been diagnosed with breast cancer so far but found to have high cancer risk. Having a strong family history of breast and/or ovarian cancer, a harmful (diseasecausing) mutation in the BRCA1 gene or the BRCA2 gene, or a high-penetrance mutation in one of many other genes associated with breast cancer risk, such as TP53 or PTEN indicates a quite high risk of breast cancer for a woman.
Bilateral prophylactic mastectomy is distinguished as the most widespread surgery for risk reduction. It may include removal of both nipples (total mastectomy) or removal of breast tissue as far as possible excluding the nipples (subcutaneous or nipplesparing mastectomy). Subcutaneous mastectomy keeps the nipples intact leading to a more natural appearance of the breast where the patient opts having breast reconstruction surgery later. Nevertheless, total mastectomy proves to be the most efficient option in risk reduction due to the fact that it removes more breast tissue than subcutaneous mastectomy [8]. The patient whose case we report choose nipple and areola spearing mastectomy out of the surgical options presented to her.
There are many factors which affect a woman’s decision to have prophylactic mastectomy. One of these factors is the perceived risk of developing breast cancer. Family history is one of the most important risk factors for developing breast cancer, because most patients with breast cancer do not have a family history and familial breast cancer accounts 10%. One of the options for preventing risk of breast cancer in women with high risk of the disease is prophylactic mastectomy. Yet, the effectiveness of prophylactic mastectomy is not known [9,10]. It was found in Geiger’s study that the occurrence of breast cancer was prevented by approximately 95% or more through bilateral prophylactic mastectomy in women cared under community practices having high risk of breast cancer [11]. It was suggested by Gail et al. that the procedure has a strong protective effect, and it is estimated that prophylactic mastectomy have prevented 15 cases of breast cancer among women of 35 years old and over when the procedure was performed [12]. The authors regarded as failure incidental breast cancers found during prophylactic mastectomy. They found a noticeable reduction in later breast cancer occurrence with the lower confidence interval at 75%. Thus, they have pointed out a clinically significant reduction in breast cancer risk following bilateral prophylactic mastectomy.
Another prophylactic option for instance is chemopreventive therapy accompanied by tamoxifen for women with high risk. The comparison prophylactic tamoxifen to placebo made by the National Surgical Adjuvant Breast and Bowel Project (NSABP) revealed that tamoxifen reduced the risk of invasive cancer by 49% during a follow-up of 55 months on average [13]. On the contrary, it was demonstrated in recent interim reports of two European trials that tamoxifen prophylaxis failed to reduce the incidence of breast cancer significantly [14,15]. One of these studies only included women with a family history of breast cancer. This contradictory data can possibly be explained by some factors such as differences in the age and risk levels of the study participants, using different numbers of patients, differences in the duration of follow-up, and the fact that in the European studies, it was allowed to use hormone replacement therapy (used by 14% in the Italian study and 41% of women in the British trial). The strength of the findings of NSABP trial is enhanced by the larger number of patients involved and the prohibition of hormone-replacement therapy.
Some aspects of single-institution study of a surgical procedure such as prophylactic mastectomy are unparalleled. Primarily, due to the specific nature of the subcutaneous mastectomy, women were referred to the Mayo Clinic particularly for the procedure. This explains why our cohort is so large. Secondarily, a limited number of surgeons performed the procedures using same techniques. This factor matters significantly in an analysis of subcutaneous mastectomy, because it is possible that the amount of retained breast tissue may vary considerably. There have been comprehensive historical indications for prophylactic mastectomy. These have included conditions that indicated no significant association with an increased risk of breast cancer [16]. Recent years have brought improvements in capability of risk prediction based on both hereditary and nonhereditary factors [17]. Thus, the capability to find out women with very high risk based on their family history or genetic analysis should contribute to making sure that this procedure is considered for the population with highest risk. The biggest reason why our patient preferred this procedure is because her mother had a breast cancer history.
The following postoperative risks must be also made clear by the surgeon;
i) Bleeding or infection,
ii) fluid accumulation under the scar,
iii) delayed wound healing,
iv) scar tissue formation, and long term risks such as;
v) prophylactic mastectomy is permanent and irreversible.
vi) this surgery leads to significant loss of feeling in the breast. This might influence sexuality.
vii) women going through prophylactic mastectomy will not be able to breastfeed from the affected breast(s) any more.
viii) some women might suffer from anxiety or depression about their body image following prophylactic mastectomy,
ix) the fact that prophylactic mastectomy may reduce the risk of breast cancer development by approximately 90% does not guarantee that breast cancer will never occur. There are cases where breast tissue extends to the collarbone and armpit which makes it impossible for a surgeon to remove all remaining cells. It is probable that breast cancer develops even in the little amount of remaining tissue.
Finally, where a woman has high risk of developing breast cancer, having a discussion with her and her family about all risk reduction options is crucial. Moreover, seeking a second opinion is quite significant for the purpose of evaluating whether prophylactic mastectomy is a procedure which contributes to her, her medical condition and life quality.
7094
References
- Willemsen HW, Kaas R, Peterse JH, Rutgers EJ (1998) Breast carcinoma in residual breast tissue after prophylactic bilateral subcutaneous mastectomy. Eur J SurgOncol24:331-332.
- Pennisi VR, Capozzi A (1989) Subcutaneous mastectromydata:a final statistical analysis of 1500 patients. Aesthetic Plast Surgery13:15-21.
- Woods JE (1986) Breast reconstruction: a current state of the art. Mayo ClinProc61:579-585.
- Garcia-Etienne CA, Borgen PI (2006) Update on the indication of the nipple sparing mastectomy. J Support Oncol4:225-230.
- Chung AP, Sacchini V (2008) Nipple-sparing mastectomy: where are we now? SurgOncol17:261-266.
- Hartmann LC, Schaid DJ, Woods JE (1999) Efficacy of bilateral prophylactic mastectomy in women with a family history of breast cancer. N Engl J Med340:77-85.
- Watson M, Lloyd S, Davidson J (1999) The impact of genetic counselling on risk perception and mental health in women with a family history of breast cancer. Br J Cancer79:868-74.
- Guillem JG, Wood WC, Moley JF (2006) Review of current role of risk-reducing surgery in common hereditary cancer syndromes. J ClinOncol. Oct 124(28):4642-60.
- Burke W, Daly M, Garber J (1997) Recommendations for follow-up care of individuals with an inherited predisposition to cancer. II. BRCA1 and BRCA2. JAMA277:997-1003.
- Hoskins KF, Stopfer JE, Calzone KA (1995) Assessment and counseling for women with a family history of breast cancer: a guide for clinicians. JAMA273:577-85.
- Ann M. Geiger, Onchee Yu, Lisa J. Herrinton(2005) A Population-Based Study of Bilateral ProphylacticMastectomy Efficacy in Women at Elevated Risk for Breast Cancer in Community Practices. Arch Intern Med.165:516-520
- Gail MH, Brinton LA, Byar DP (1989) Projecting individualized probabilities of developing breast cancer for white females who are being examined annually. J Natl Cancer Inst.81:1879-1886.
- Powles T, Eeles R, Ashley S (1998) Interim analysis of the incidence of breast cancer in the Royal Marsden Hospital tamoxifen randomised chemoprevention trial. Lancet352:98-101.
- Powles T, Eeles R, Ashley S (1998) Interim analysis of the incidence o breast cancer in the Royal Marsden Hospital tamoxifen randomised chemoprevention trial. Lancet352:98-101.
- Veronesi U, Maisonneuve P, Costa A (1998) Prevention of breast cancer with tamoxifen: preliminary findings from the Italian randomised trial among hysterectomised women. Lancet352:93-7.
- Pennisi VR. (1986) Redefined indications for subcutaneous mastectomy in patients with benign breast disease. Aesthetic PlastSurg10:101-4.
- Couch FJ, DeShano ML, Blackwood MA (1997) BRCA1 mutations in women attending clinics that evaluate the risk of breast cancer. N Engl J Med336:1409-15.






