Orugbo VP1*, Ohaju-Obodo J2, Ochei O3 and Ntaji MI3
1Department of Chemical Pathology, Delta State University, Abraka, Delta State, Nigeria
2Department of Internal Medicine, Delta State University, Abraka, Delta State, Nigeria
3Department of Community Medicine, Delta State University, Abraka, Delta State, Nigeria
- Corresponding Author:
- Orugbo Peter
Department of Chemical Pathology
Delta State University, Abraka, Delta State, Nigeria
Tel: 2348036899761
E-mail: drorugbopeter@gmail.com
Received date: August 03, 2020, Accepted date: August 21, 2020, Published date: August 28, 2020
Citation: Orugbo VP, Ohaju-Obodo J, Ochei O, Ntaji MI (2020) Degree of Completion of Laboratory Request Forms in a Tertiary Hospital in Nigeria. Acta Psychopathol Vol.12 No.5:28. DOI: 10.36648/1989-5216.12.5.329
Keywords
Completion; Laboratory form; Nigeria
Introduction
Request forms from the laboratory constitute vital communication piece between laboratory personnel and managing physicians who depend on results generated from the laboratory for patients management and efficiency [1,2]. Reports from studies show that information generated from the laboratory has a profound impact on patients diagnoses and wellness: laboratory report constitute between 60-70% of useful clinical information needed in the management of both in-patients and out-patients in hospital setting [3,4].
Biochemical reports are interpreted and reported by chemical pathologists; who are trained medical doctors. Pathologists require patients’ biodata, clinical presentations and laboratory findings to reach agreeable conclusion in patients’ diagnosis and treatment [5-7]. The importance of adequate completion of request forms is usually underestimated by physicians who may result in poor ability of pathologist to correctly interpret results; wrong allocation and delivery of patients’ resultsleading to delay in instituting prompt treatment [8-13]. Delay in instituting treatment is dangerous particularly in case of highly communicable infectious disease- may result in outbreak of the disease-disrupting public health. Inadequately filled form is of no good in epidemiological studies.
In most studies the only variables provided by requesting clinicians on laboratory request forms were the patients name and the test to be conducted. Exclusions in laboratory request forms as identified and reported in the literatures are being classified in these formats: scanty information on patient’s sociodemographic characteristics (name, age, sex, address, ward, laboratory number); insufficient information on the test to be done (name of the sample, fasting status of the patient), scanty or no clinical information, and omission of requesting physician name (doctor’s name, phone number and signature) and contact, and unreadable letters [14].
The age of the patient would provide useful information to the pathologist in the interpretation of most biochemical specimens: premenopausal women have higher “High Density Cholesterol Lipoprotein” than post-menopausal women. Pregnant women and children have higher alkaline phosphatase levels than the general population. Some samples like serum cortisol, fasting plasma glucose and fasting serum lipid profile need date and most especially time of collection for their interpretation. Cortisol values fluctuate (diurnal rhythm) throughout the day. Biochemical values differ in men and women. The contact of the referring doctor is vital in emergency situations and for immediate contact and clarification of information on the request form. From these perspectives; complete and correctly filled laboratory request forms have a colossal impact on the quality of results generated from the laboratory, and in turn have greater impact in patients’ treatment, improvement and general well-being. On the contrary, when laboratory request forms are inadequately completed, there will be fragmentary and erroneous pathologists’ advice to clinicians [8-14]. Evidence from studies showed that pre-analytical errors now constitute the major errors in laboratory testing, and inadequately completed request forms contribute most to preanalytical errors [8-14].
Hence, experts have suggested that health institutions should periodically audit “work processes” against measurable criteria to ascertain gaps, and to recommend corrective measures to improve patient care and wellbeing [15]. As clinicians’ responsibilities are getting more diverse, their tendencies to complete routine tasks become derisive; still they need to embrace the tradition of adequately filling a laboratory form which relies strongly on the health institution.
On this note, the study audited the level of completion of request forms presented to the Chemical Pathology Department of a University Teaching Hospital in Nigeria. The fundamental findings in this study will be disseminated to the hospital management, which will help institute control measures.
Research Methodology
Study setting
The study was conducted in Delta State University Teaching Hospital (DELSUTH), Oghara, Delta State, Nigeria. DELSUTH is a renowned and accredited university teaching hospital to the Delta State University (DELSU), Abraka. The institution is located in Oghara, Ethiopia West Local Government Area of Delta State. The hospital, a 180-bed ultra-modern specialist hospital was built to provide quaternary services to the indigenes of Delta State and its neighbours. An inaugural management board was sworn in June 2009 to manage the affairs of the hospital when it kickedoff. The earliest staff of DELSUTH consisted of a team of qualified Nigerian medical professionals drawn from the United Kingdom and the United States. The hospital was officially commissioned on the 19th of June, 2010 [16].
The study was conducted in the Department of Chemical Pathology of the hospital. There are ten (10) scientists, five (5) laboratory technicians and one chemical pathologist in the department. The chemical pathologist is the lead investigator in this study. The department has state of the art medical equipment: Lian Abbott architect auto analyzers (architect i1000SR for immunoassays) and architect c4000 for electrolytes and other chemical analytes. These machines work on the principles of electro-chemiluminescence and immunochemistry assays. There are also back up machines, like ERBA auto analyzer and electrophoresis machine.
The department provides biochemical services to the hospital and environs. Services are run 24 hours and staff run shift. Out patients samples are collected in the phlebotomy centre, while ward samples are collected from wards by doctors. Samples are brought to the laboratory by porters. Laboratory scientists carry out investigations, assisted by laboratory technicians. The scientist training also includes how to use the machines and carry out chemical analyses. Technicians assist with preparations like centrifuging samples; lab recordings, and needed errands in the laboratory. Chemical Pathologists report results using the results generated by the scientists with the information in the laboratory in the request forms especially clinical details.
Study design
The study is a retrospective cross-sectional study.
Study population and sampling strategy
Laboratory Request Forms (LRFs) submitted to the Department of Chemical Pathology by hospital clinicians, from October 2019 to December 2019 were reviewed systematically and assessed for correctness and completeness. The requesting clinicians were not aware that forms submitted to the laboratory were assessed for completeness. The minimum sample size was 290 estimated by Fischer’s method.
Data collection
A SPSS master sheet containing all the variables (hospital number, patient name, patient sex, patient age, patient address, patient contact number, ward/clinic, consultant name consultant contact, laboratory form signed by doctor; type of sample collected, investigation requested, date sample was received by the laboratory; time sample was collected, date and high risk sample) indicated in the laboratory request forms were produced to collect the information in the forms.
Data analysis
Each patient laboratory request form was coded using Arabic numerals before entering into the sheet. The entering and analysis was done by a data analyst using SPSS version 25, and validated by one of the researcher to ensure there were no wrong entries. The results were presented as frequency tables. A form was said to be completely filled if it had all the information indicated in the form.
Ethical considerations
Ethical clearance was obtained from the Delta State University Teaching Hospital, Oghara.
Results
Table 1 show the parameters filled in the laboratory form.
| Variables |
Frequency (n=291) |
Percent (%) |
| Patient name |
291 |
100 |
| Patient sex |
290 |
99.7 |
| Patient age |
231 |
73.4 |
| Patient address |
150 |
51.5 |
| Hospital number |
201 |
69.1 |
| Patient contact number |
0 |
0 |
| Ward/clinic |
285 |
97.9 |
| Consultant name |
257 |
88.3 |
| Consultant contact |
| Lab form signed by doctor |
283 |
97.3 |
| Type of sample collected |
149 |
51.2 |
| Investigation required |
291 |
100 |
| Date received by the lab |
0 |
0 |
| Time sample was collected stated |
22 |
7.6 |
| Date lab form was filled |
290 |
99.7 |
| High risk sample |
19 |
6.5 |
| Forms completely filled |
0 |
0 |
Table 1: Parameters indicated in the laboratory form by requesting physician.
A total of 291 forms received during the study period in which 291 (100%) forms indicated patient name, 290 (99.7%) forms indicated patient sex, 231 (73%) indicated age, 150 (51.5%) indicated patients’ address, and 201 (69.1%) forms indicated hospital number. None indicated the patients contact number, 285 (97.3%) indicated the ward, and 257 (88.3%) indicated the consultant name; 283 (97.3%) of the forms were signed by the doctor. About 291 (100%) and 149 (51.2%) forms indicated the investigation to be carried out and sample collected respectively. None of the forms indicated the date received by the laboratory, 22 (7.6%) and 290 (99.7%) of the forms indicated time and date sample was collected respectively, while 19 (6.5%) of the lab form indicated if it was a high risk sample. All the laboratory forms were not completely filled.
Figure 1 shows the level of inadequacy: 208 (71.5%) of the laboratory forms indicated 5 to 9 parameters while 83 (28.5%) indicated 10 to 16 parameters.
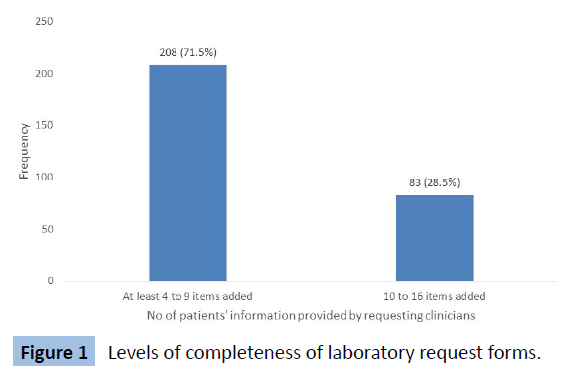
Figure 1: Levels of completeness of laboratory request forms.
Discussion
It is the mandate of the requesting physician to completely fill in required information in laboratory request form before sending to the laboratory for specimen analysis because pathologists need to correlate information in the request form and results of tests ran in the laboratory to make utmost input in patients’ diagnoses and management. Perceptively, this study was conducted to clarify the readiness of requesting physicians completely filling required information in laboratory request forms. Sadly, none of the forms received during the study period was completely filled. The only information provided always in all the forms were patients name and test requested by physicians. Patients’ contact number and the date the sample was collection were omitted in all the forms. The other information provided by most physicians were patients’ sex, wards, consultant name, requesting doctor signature (for consultant) and date of request. Most forms do not have the time sample was collected and if sample was high risk. The reasons for the difficulty in completing filling forms and persistent omission of some parameters are often attributed to lack of time. Doctors may have time to clerk and document in patients case-notes, but have no time to properly or completely fill laboratory request forms. Medical students may not actually have been taught by their teachers on the significance of completely filling laboratory request forms, or even when properly taught, do not still adequately fill laboratory request forms when they become doctors, perhaps due to lack of time excuse also. Efforts need to be put in place now to combat this error.
Seemingly, most previous studies are more or less in support of this study result; the degree of completion of laboratory request forms range from 0.1-14.7% [2,3,12,13,17,18]. Only one study reported over 80% forms completed. Patient’s name was found in all laboratory request forms in almost all the studies reviewed; while the test requested was omitted in just a few of the laboratory request forms in the studies reviewed [1,2,4,11- 13,17-19].
Conclusion
Adequate measures should be taken to develop a concrete win in the subject matter – reorientation and some discipline on the part of physicians may positively accelerate the process of completion and adequacy in the filling of laboratory request forms.
Conflict of Interest
The authors declared that they have no competing interests.
32856
References
- Jegede F, Mbah HA, Dakata A, Gwarzo DH, Abdulrahman SA, et al. (2016) Evaluation laboratory request forms submitted to haematology and blood transfusion departments at a hospital in Northwest Nigeria. Afr J Lab Med 5: 381.
- Kipkulei JC, Lotodo TC (2019) Evaluation of the completeness in the filling of laboratory request forms submitted to the haematology laboratory at a tertiary hospital in kenya. Health 11: 862-868.
- Nutt L, Zemlin AE, Erasmus RT (2008) Incomplete laboratory request forms: the extend and impact on critical results at a tertiary hospital in South Africa. Ann Clin Biochem 45: 691-6987.
- Olayemi E, Asiamah-Broni R (2011) Evaluation of request forms submitted to the heamatology laboratory in Ghanaian tertiary hospital. Pan African Medical Journal 8: 33.
- Marshall WJ, Challand GS (2000) Provision of interpretative comments on biochemical report forms. Ann Clin Biochem 37: 758-763.
- Osegbe ID, Afolabi O, Onyenekwu CP (2016) Completion of laboratory test request forms at a tertiary hospital. Ann Med Health Sci Res 6: 90-94.
- Burnett L, Chesher D, Mudaliar Y (2004) Improving the quality of information on pathology request forms. Ann Clin Biochem 41: 53-56.
- Carraro P, Plebani M (2007) Errors in a stat laboratory: types and frequencies 10 years later. J Clin Pathol 53: 1338-1342.
- Plebani M (2006) Errors in a clinical laboratories or errors in laboratory medicine? Clin Chem Lab Med 44: 750-759
- Plebani M, Carraro P (1997) Mistakes in a stat laboratory: types and frequency. Clin Chem Lab Med 43: 1348-1351.
- Adegoke OA, Idowu AA, Jeje OA (2011) Incomplete laboratory request forms a contributory factor to preanalytical errors in a Nigerian teaching hospital. African Journal of Biochemistry Research 5: 83-85.
- Forae GD, Obaseki DE (2017) Adequacy of clinical information supplied by clinicians for histopathologic diagnosis: the university of Benin teaching hospital experience. N Niger J Clin Res 6: 12-15.
- Adizua UC (2019) Incomplete filling of laboratory request forms: a look at the practice at a federal medical centre in South Eastern Nigeria. West African J Med 36: 112-115.
- Onyiaorah IV, Ukah CO, Anyiam DCD, Odike MAC, Oyeka ICA (2012) Effect of remedial measures on inadequacies in the completion of request forms by clinicians. Clinical Audit 4: 9-14.
- National Institute for Clinical Excellence (2002) Principles for best practice in clinical audit. London: National Institute for Clinical Excellence.
- IBM Corp (2017) IBM SPSS Statistics for Windows, Version 25.0. Armonk, NY: IBM Corp.
- Manoharan K, Manoharan H, Sharma C (2019) Evaluation of laboratory request forms submitted to clinical pathology department in a tertiary hospital. Int J Res Med Sci 7: 2399-2402.
- Adamu S. Mohammed A, El-Bashir JM, Abubakar JD, Mshella DS (2018) Incomplete patient data on chemical pathologist forms in a tertiary hospital in Nigeria. Ann Trop Pathol 9: 47-49.
- Oladeinde BH, Omoregie R, Osakue EO, Onifade AA (2012) Evaluation of laboratory request forms for incomplete data at a rural tertiary hospital in Nigeria. NZ J Med Lab 66: 39-41.







