Fuat IpekcBekir Ozenen, Gökdeniz Ceren Ozenen, Muharrem Karaoglan and Ismail Sert
1Tepecik Training and Research Hospital, izmir Turkey
2Bakent University, Faculty of Medicine, Ankara,Turkey
*Corresponding Author:
Fuat Ipekc
Tepecik Training and Research Hospital
izmir Turkey
E-mail: doktor.ipek@hotmail.com
Introduction
Gallstone ileus is responsible for 1-4% of all cases with smallbowel obstruction [1,2]. Cholecystoduodenal fistula is a rare clinical entity resulting from the inflammation of the gallbladder [3]. Preoperative diagnosis of the cholecystoduodenal fistula is diffucult due to the obscure clinical picture. In general, diagnosis is established intraoperatively.
We present a case of cholecystopyloric fistula caused intestinal obstruction with interesting CT findings and successful treatment in one stage operation.
Case Report
A 66-year-old female was admitted to the hospital with abdominal pain. She had acute onset of nausea, vomiting, abdominal pain, distension and constipation. Clinical examination revealed abdomen with bloating, diffuse tenderness. There was no rebound and defense. Laboratory findings included a white blood cell count of 6.2 cells/nL,a platelet count of 268 cells/nL, a hemoglobin of 11.8 gr/dl, a blood urea nitrogen of 54 mg/dl, a potassium of 3.1 mmol/L.
Abdominal x-ray demonstrated air-fluid levels originated from the small intestine in the upper abdomen (Figure 1). Computed Tomography (CT) scan revealed perforation of the gallbladder, pneumobilia in the common duct and intrahepatic biliary tract compatible with fistula and distention of the stomach (Figures 2 and 3). The patient underwent operation with the diagnosis of ileus and acute abdomen. In the operation, the gallbladder was fistulized into the gastric pylorus wall. It was observed multiple adhesions between small bowels. A gallstone in a diameter of 25- 30 mm that caused the obstruction at distance of 70 cm from ileocecal valve was found. All small bowels were distended. The impacted gallstone was removed by enterotomy. A Kocher's maneuver was performed. The cholecystopyloric fistula were identified. Cholecystectomy and excision of the fistula was performed. Pyloroplasty and truncal vagotomy, excision of the fistula and cholecystectomy were performed. Post operative patient’s follow up was uneventful.
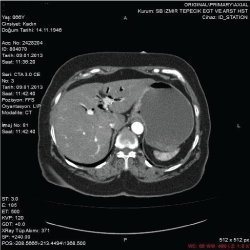
Figure 1: Air-liquid levels in small bowel segments.
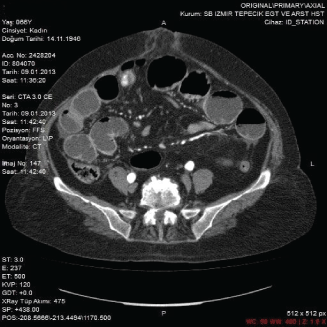
Figure 2: Gallstone in a diameter of 2.5 cm localized in distal segment of ileum, dilatation of proximal intestinal segments and distention of the stomach.
Figure 3: Pneumobilia in CT scan.
Discussion
Mechanical bowel obstruction due to gallstones are very rare, (1- 4%) [4]. Cholecystoenteric fistula occur in less than 1% of patients with gallstones. Sixty% of them are cholecystoduodenal fistula, but cholecystocolic, cholecystogastric and choledochoduodenal fistula have been also described [2,5]. Pericholecystic inflammation after cholecystitis, as well as pressure necrosis by the gallstone against the biliary wall may lead to form of a biliary enteric fistula [4]. Large stones passing through the fistula may cause intestinal obstruction, especially in the terminal ileum [2,5]. If the gallstone is located in the distal stomach or proximal duodenum and leads to gastric obstruction, this phenomenon is called as Bouveret syndrome. In this case report, A rare form of cholecystoenteric fistula, cholecystopyloric fistula was observed.
CT may demonstrate pneumobilia, intestinal obstruction and ectopic gallstone [5]. The classic radiological Rigler's triad which includes mechanical intestinal obstruction, pneumobilia and ectopic gallstone in the intestinal lumen has to investigated [6]. The presence of air in the gallbladder and pneumobilia are common findings in cases with gallstone ileus [6,7]. Abdominal x-rays and ultrasound are not usually sufficient [6]. In recent years, by the help of CT scan, diagnosis of the cholecystoenteral fistulas are gradually increasing but the percentage of patients diagnosed at laparotomy remains high [6]. The best imaging technique to identify the elements of the Rigler triad is CT. The diagnosis by CT is possible in 75% of cases [2,8]. CT could also depict the biliodigestive fistula [2].
The optimal treatment of patients with cholecystopyloric fistulas still remains controversial [2]. Possible strategies are a one-stage approach with enterotomy, cholecystectomy and resection of the fistula at once, or a two-stage approach with an emergency enterotomy to remove the obstructing gallstone and cholecystectomy and fistula resection in the second operation. It seems a reasonable to restrict the one-stage approach to clinically stable patients and choose a two-stage approach in patients with severe cholecystitis and high perioperative risk as a result of concomitant comorbidities [4].
Open surgery, endoscopic removal and laparoscopic enterolithotomy have been attempted for stone removal [1,7]. Many authors support cholecystectomy and fistula repair during the first [2] or second operation depending on the general status of the patient and the local findings [2].
In 1929, Holz was the first one who performed cholecystectomy and fistula repair. In 1972, Redding et al. performed vagotomy and Jaboulay gastroduodenostomy in a patient with impaction of two gallstone, one in the antrum and another in the duodenal bulb, and a very extended local inflammation [2]. In our patient,the impacted gallstone in the ileum was removed by enterotomy. The cholecystopyloric fistula was identified. Cholecystectomy and excision of the fistula was performed. Pyloroplasty (Heineke- Mikulicz) and truncal vagotomy with excision of the fistula followed by cholecystectomy were performed.
Conclusion
A CT scan of the abdomen could be helpful in diagnosis of cholecystopyloric fistula and gallstone ileus. If the patient’s medical condition is stable and suitable, a one-stage surgical approach with simultaneous enterotomy, cholecystectomy and fistula resection is feasible.
Disclosure
This case has been presented as a poster in the 9. National Trauma and Emergency Surgery Congress of Antalya (19-23 april,2013).
7096
References
- Algin O, Özmen E, Metin MR, Ersoy PE, Karaoglanoglu M (2013)Bouveretsyndrome:evaluation with multidetector computed tomography and contrast-enhanced magnetic resonance cholangiopancreatography.Turkish Journal of Trauma&Emergency Surgery19:375-379.
- Mavroeidis VK, Matthioudakis DI, Economou NK, Karanikas ID (2013)Bouveret syndrome-The rarest variant of gallstone ileus:A case report and literature review.Case Reports in Surgery.
- Yüksel O, Sakrak Ö, Tatlicioglu E, Sahin T, Bostanci H (2007)Cholecystoduodenal fistulae:Report of three cases.Turkish Journal of Surgery 23:069-072.
- Giese A, Zieren J,Winnekendonk G, Henning BF (2010) Development of a duodenal gallstone ileus with gastric outlet obstruction(Bouveret Syndrome) four months after succesful treatment of symptomatic gallstone disease with cholecystitis and cholangitis:A case report. J Med Case Rep23:376-382.
- Masannat YA, Caplin S, Brown T (2006) A rare complication of a common disease: Bouveret syndrome, a case report.World J Gastroenterol 12: 2620-2621.
- Gerzilov P, Sedloev T, Penkov N, Asenov Y, Golemanov B, et al. (2014) A rare combination between Bouveret's syndrome and upper intestinal obstruction.Causapedia3:741-745.
- Reisner RM, Cohen JR (1994) Gallstone ileus: a review of 1001 reported cases.Am Surg 60: 441-446.
- Shah SK, Walker PA, Fischer UM, Karanjawala BE, Khan SA (2013) Bouveret syndrome.J GastrointestSurg 17: 1720-1721.








