Keywords
Hepatit B virus; HBV serologic level; Anti-HCV; Anti-HAV
Introduction
Hepatitis B virus (HBV) is a DNA virus of the family Hepadnaviridae. Its specific areas in body are limited and they can cause deadly diseases like acute infection, persistent infection, fulminant hepatitis, cirrhosis and hepatocellular carcinoma where they settled [1].
HBV infection is common in the world and is a major public health problem and in case of chronic, it can lead to serious complications such as cirrhosis, reinfection and carcinoma [2-4]. It causes mortality and morbidity at a considerable extend. It has been informed that approximately 400-500 million people around the world, in our country of 3 million people is a carrier of HBV infection and this infection results in approximately the death of 1-2 million people worldwide each year [5-7]. Healthcare staff has a higher risk in terms of contamination and spread of viral, bacterial, fungal and protozoonal diseases compare to other segments of society. In this regard, hospital employees should be taught the ways of protection from viral hepatitis and vaccination programs should be implemented. So you would have taken precautions against HBV and a reduction in complications occurs depending on the HBV can be observed [8].
In acute infections, the first virus antigen detected in blood is HBsAg. 4-6 weeks after receipt of the virüs, it is detected in the blood [9]. In acute infections, HBs Ag can be seen serological tests up until the sixth month. If it lasts more than 6 months, it indicates that it has become chronic [10]. The presence of HBe Ag indicates that viral replication continues. During this period, HBe Ag DNA Polymerase can be determined and this period is called the window period [9]. After 1-4 weeks of HBs Ag detection, an increase is seen in Anti-HBc IgM (Figures 1 and 2). The determination of IgM anti-HBc indicates that reduced viral replication. It indicates the improvement of the disease towards better. The continued existence of Anti-HBc IgM in the serum indicates that the disease is chronic [10]. Anti HBs shows up just after HBs Ag vanish in serum. In fact it is acknowledged that Anti HBs Ag occurs earlier; but immune complexes that occur in excess of HBs Ag suppress it. 1 or 2 weeks after HBe Ag vanishes, Anti-HBe is detected in serum [9]. The existence of HBs Ag more than 6 months and the existence of HBc IgM in serum for a long time indicate that the disease is chronic [10].
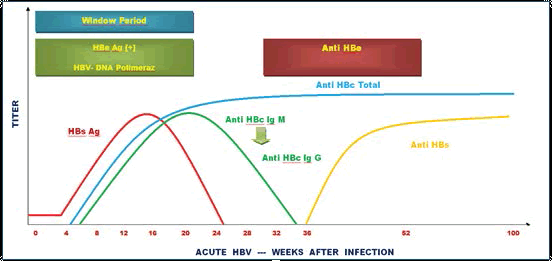
Figure 1: Acute HBV or changes in serological data depending on weeks.
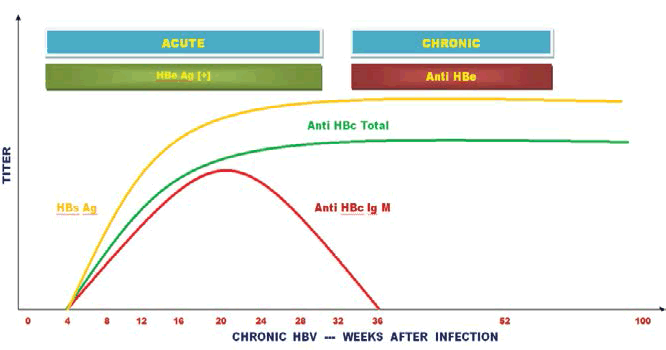
Figure 2: Chronic HBV or changes in serological data depending on weeks.
Material and Methods
A total of 113 dentistry students aged 20-25 years were invited to participate in the study. The health examination at study entry included serological tests for HBS Ag, Anti HCV, Anti HAV ve Anti HBc. Serological markers were determined by ELISA test. Serological marker results retrospectively were analyzed and statistical analyses were assessed by Statistical Package for the Social Sciences (SPSS) 21.
Results
In the results of ELISA of 113 people including 58 women and 55 men, HBsAg Macro, Anti-HCV Macro, anti-HBs Macro, anti- HIV, Anti-HAV Ig G values were examined while analyzing macro values. The macro-HBs HBS value of a female student was found to be greater than 1 and HBV-positive was diagnosed (Table 1).
| Valid |
Frequency |
Percent |
Valid Percent |
Cumulative Percent |
| 000 |
1 |
0,9 |
0,9 |
0,9 |
| 010 |
1 |
0,9 |
0,9 |
1,8 |
| 050 |
2 |
1,8 |
1,8 |
3,5 |
| 060 |
2 |
1,8 |
1,8 |
5,3 |
| 080 |
1 |
0,9 |
0,9 |
6,2 |
| 100 |
3 |
2,7 |
2,7 |
8,8 |
| 110 |
2 |
1,8 |
1,8 |
10,6 |
| 120 |
2 |
1,8 |
1,8 |
12,4 |
| 130 |
3 |
2,7 |
2,7 |
15,0 |
| 140 |
10 |
8,8 |
8,8 |
230,9 |
| 150 |
11 |
9,7 |
9,7 |
33,6 |
| 160 |
13 |
11,5 |
11,5 |
45,1 |
| 170 |
11 |
9,7 |
9,7 |
540,9 |
| 180 |
7 |
6,2 |
6,2 |
61,1 |
| 190 |
7 |
6,2 |
6,2 |
67,3 |
| 200 |
7 |
6,2 |
6,2 |
73,5 |
| 210 |
6 |
5,3 |
5,3 |
78,8 |
| 220 |
2 |
1,8 |
1,8 |
80,5 |
| 230 |
2 |
1,8 |
1,8 |
82,3 |
| 240 |
2 |
1,8 |
1,8 |
84,1 |
| 254 |
1 |
0,9 |
0,9 |
85,0 |
| 260 |
1 |
0,9 |
0,9 |
85,8 |
| 280 |
1 |
0,9 |
0,9 |
86,7 |
| 290 |
1 |
0,9 |
0,9 |
87,6 |
| 310 |
1 |
0,9 |
0,9 |
88,5 |
| 340 |
1 |
0,9 |
0,9 |
89,4 |
| 380 |
1 |
0,9 |
0,9 |
90,3 |
| 400 |
1 |
0,9 |
0,9 |
91,2 |
| 440 |
1 |
0,9 |
0,9 |
92,0 |
| 450 |
1 |
0,9 |
0,9 |
920,9 |
| 470 |
1 |
0,9 |
0,9 |
93,8 |
| 521 |
1 |
0,9 |
0,9 |
94,7 |
| 630 |
2 |
1,8 |
1,8 |
96,5 |
| 692 |
1 |
0,9 |
0,9 |
97,3 |
| 716 |
1 |
0,9 |
0,9 |
98,2 |
| 750 |
1 |
0,9 |
0,9 |
99,1 |
| 47,61,190 |
1 |
0,9 |
0,9 |
100,0 |
| Total |
113 |
100,0 |
100,0 |
|
Table 1: The results of HBsAg MACRO values. Reference range for this value is “>1 positive”. As the unit, it is expressed as S/CO.
When Anti-HCV values were analyzed, the HBs macro value of 110 students is less than 1. This means that students have no immunity against HCV. In further laboratory results of 3 students, Anti HCV values were not shown. Regarding Anti HBS value in further laboratory results, A person was found to be 0 mIU/ml, 10 persons had 0-10 mIU/ml, 79 persons found to be between 10 and 1,000 mIU/ml, and 23 people were found to be greater than 1000 mIU/mL (Table 2). These values were charted with IBM SPSS Statistics (Figure 3). While analyzing value of Anti-HIV of serological markers, the value of the anti-HIV of 24 students was found to be less than 1. These students were identified not to have any immunity against HCV. In the Elisa test results of 89 students, the results belonging these markers were not detected. When Anti HAV values of serological markers were analyzed, 23 students were identified that somehow or other they encountered with the hepatitis A virüs. In further laboratory results of 60 students, a Anti-HAV related result was not found. Anti-HAV serologies of 30 students were found below 1.
| Valid mIU/mL |
Frequency |
Percent (%) |
Valid Percent% |
Cumulative Percent % |
| 0 |
1 |
,9 |
,9 |
,9 |
| 0-10 |
10 |
8,8 |
8,8 |
9,7 |
| 10-1000 |
79 |
69,9 |
69,9 |
79,6 |
| >1000 |
23 |
20,4 |
20,4 |
100,0 |
| Total |
113 |
100,0 |
100,0 |
|
Table 2: Anti HBS case markers to be shown as pie charts with IBM SPSS Statistics.
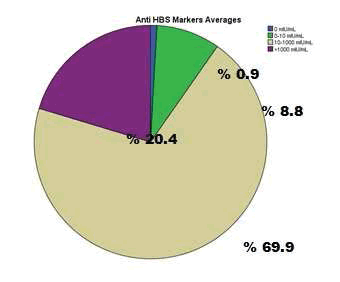
Figure 3: Showing anti HBS markers with pie chart obtained via IBM SPSS Statistics.
Discussion
Just because health care staff has a close contact with patients, when they perform their professional responsibilities, they need to have sufficient knowledge about HBV infection in order to protect themselves [11]. The prevalence of HBV markers in health care workers is mostly related to the contact rate with blood rather than being in contact with the patient. For this reason, it has been informed that in addition to the doctors and nurses who are in face-to-face contact with patients, the other staff working in hospital have the same risks [12,13]. Isikgöz et al., in one of their study, informed that more than half of the staff in a hospital can be contaminated HBV and HCV by means of saliva and extracorporeal fluids other than blood [14]. The risk of transmitting HBV by a skin contact with the blood of a person who has positive HBe Ag to someone else has been found to be 30% [15].
Acute HBV infection can be symptomatic or asymptomatic. Because the majority of cases are asymptomatic, it is usually not detectable in the acute stage. A large proportion of clinical findings can be followed without hospitalization. There is no specific treatment for acute HBV, but the patient is recommended to rest. Until there is improvement in clinical and biochemical data, alcohol intake, use of analgesics, sedatives and hepatotoxic drugs should be prohibited. Liquid supplements should be made in patients with severe vomiting. Severe nausea, vomiting, mental changes, should be monitored in the hospital for patients with encephalopathy [16].
In the treatment of chronic HBV, interferon alfa-2a and 2b, pegylated interferon alfa-2a and 2b, lamivudine, adefovir, entecavir, and tenofovir are present in our country and are user-approved drugs. HBV-infected pregnant women should be evaluated for hepatic flare.
When ELISA test results are taken into consideration, the preclinical and clinical students were found to have insufficient knowledge about markers. After giving the necessary information about hepatitis infection to preclinical and clinical students, they have been proposed to routinely control hepatitis markers.
Conclusion
The presence of HBsAg in the serum is determined by ELISA method. Analytical errors during the test, the contamination, anticoagulated samples related to ELISA method can cause false positive reactions. Therefore, the HBsAg positivity should be verified with other serological parameters like anti-HBc. Trainee students are mostly educated in vaccination against HBV and they know enough about the status of the immune response of themselves; yet, they have been identified not taking the necessary measures while examining the patients. Trainee students should be trained about HBV at regular intervals. All health care workers and personnel should be vaccinated against HBV.
9108
References
- Mandell GL, Bennet JE, Dolin R (2000) Mandell Douglas and Bennet’s Principles and Practice of Infectious Diseases. 5th ed. New York, Churchill Livingstone 135.
- Yu MW, Chang HC, Liaw YF (2000) Familial risk of hepatocellular carcinoma among chronic hepatitis B carriers and their relatives. J Natl Cancer Inst 92: 1159.
- Shepard CW, Simard EP, Finelli L, Fiore AE, Bell BP (2006) Hepatitis B virus infection: Epidemiology and vaccination. Epidemiol Rev 28: 112-125.
- Stiffel TA, Mandell GL, Bennett JE, Dolin R (2000) Principles and Practice of Infectious Diseases. 5th ed. Churchill Livingtone 1297-1331.
- Margolis HS, Last JM, Wallace RB (1992) Maxcy-Rosenau-Last Public Health&Preventi Medicine. 13th ed. East Norwalk: Appleton& Lange 131- 139.
- Willey JM, Sherwood LM, Woolverton CJ (2011) Human diseases caused by viruses and prions, Direct contact diseases: Viral hepatitides. In: Prescott's Microbiology. International Edition. Eighth Edition. New York: The McGraw Hill Companies 919-921.
- Çetin M, Temiz M, Aslan A (2007) Determination of the Knowledge Levels on Hepatitis B Virus of Residents at Mustafa Kemal University Hospital 12: 121-127.
- Centers for Disease Control and Prevention (1997) Immunization of health careworkers: Recommendations of the Advisory Committee on Immunization 46: 1-42.
- Shapiro CN (1993) Epidemiology of hepatitis B. Pediatr Infect Dis 12: 433–437.
- Centers for Disease Control National Institute for Occupational Safety and Health (2000) Science and public health issues that pertain to needlestick injuries among health care workers.
- MMWR (1991) Recommendations for preventing transmission of human immunodeficiency virus and hepatitis B virus to patients during exposure-prone invasive procedures 40: 1-9.
- Curry MP, Chopra S (2005) Acute Viral Hepatitis. Principles and Practice of Infectious Diseases. 6 ed. Philadelphia: Churchill Livingstone 1426-1441.
- Mahoney FJ (1999) Update on diagnosis, management, and prevention of hepatitis B virus infection. Clin Microbiol Rev 12: 351-366.








