Sadichha Thapa1*, Abu Taiub Mohammed Mohiuddin Chowdhury2 and Sedzro Divine Mensah3
1Department of Gynecology & Obstetrics, The1st affiliated Hospital of Jiamusi University, China
2Department of Digestive disease-II, The 1st affiliated Hospital of Jiamusi University, China
3Department of Laboratory Medicine, The 1st affiliated Hospital of Jiamusi University, China
*Corresponding Author:
Sadichha Thapa
Department of Gynecology & Obstetrics
The1st affiliated Hospital of Jiamusi University
China
E-mail: tsadichha@gmail.com
Introduction
Rudimentary uterus is one of the rarest gynecological anomalies. Due to the wide variation of the presentation, this clinical condition remains as an interesting point of study regarding the diagnosis and challenges of management. Evaluation of a rudimentary uterine horn in young patients is very less reported among the published literatures.
Case Report
We report a 14 years old female patient presented in the outpatient Gynecology department of 1st affiliated hospital of Jiamusi University on 13th October with a History of severe lower abdominal pain for a period of 4 days. She described the pain as continuous in type with no aggravating factor. She was menarche at the age of 13 years with H/O Dysmenorrhoea, regular menstrual cycle of 30 days and an average duration of 7 days high menstrual flow. On examination the patient was generally healthy. Her lower abdomen was soft and tender. Notable tenderness was detected in the left iliac fosse. Bowel sound was normal. She denied weight loss, history of fever, vomiting, altered bowel habit and Dysuria. No major systemic illness was detected. She had a short history of NSAID intake for 4 days with no history of Allergy, previous surgical intervention and medical illness. She was non Diabetic and non-Hypertensive with no history of smoking and alcohol.
Her routine blood and urine test were normal. The ultrasound examination reveals a pelvic mass in the left adnexal region and significant collection in the posterior fosse with an advice for clinical correlation (Figure 1).
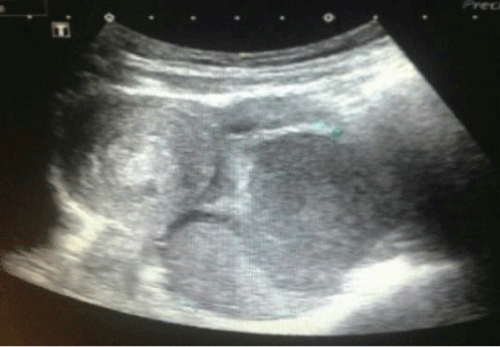
Figure 1: Transvaginal ultrasound showing a solid hypo echoic area just left to the uterus, with a differential diagnosis of solid left adnexal mass.
As the pain was increasing, after consultation with informed consent a laparoscopic evaluation under general anesthesia was performed. The approach was made through the umbilicus and a thorough examination of the pelvic organs was done. Laparoscopic examination reveals abnormal development of the reproductive organs and a cyst in the left ovary of about 9 cm in size (Figure 2).
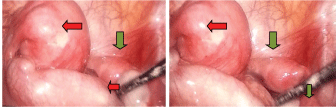
Figure 2: Laparoscopic examination showing the uterus (leftarrow marked), the rudimentary uterus (Right arrow marked) and the Left ovary in the tip of the artery stick.
Following developmental anomalies were detected in her reproductive organs:
Two separate uteri were identified. The left uterus was of 8 x 6 x 6 cm in size and linked to left accessory organ with abnormal development. No fimbrae was noted in the left side which was linked to the left ovary with a large cyst of about 9 cm in size at the end of the fallopian tube. The anterior wall of the left uterus was adherent with the pelvic wall forming a concealed area filled with altered hemorrhage. During separation which burst out with oozing of blood. The right uterus was 3 x 3 x 2 cm in size and was linked to right ovary and fallopian tube. Both the uterus was attached by a wide ligament with no evidence of opening or continuation between them. With further consent laparotomy was performed. The left ovarian cyst was drained and excised; it was filled with chocolate color fluid. During the operation procedure confusion arose with the rudimentary horn of the uterus. So vaginal examination was performed and a dilator was used for exploration. The cervix was found to be continuous with the right uterus. The left uterus was diagnosed as rudimentary horn and was excised along with the fallopian tube and ovary attached to it (Figure 3). Homeostasis was maintained. Vagina was observed a little lacerated at 11 and 3o’clock position of hymen of introitus and was sutured with absorbable material. Histological confirmation was done for the excised segment of the uterus (Figure 4).
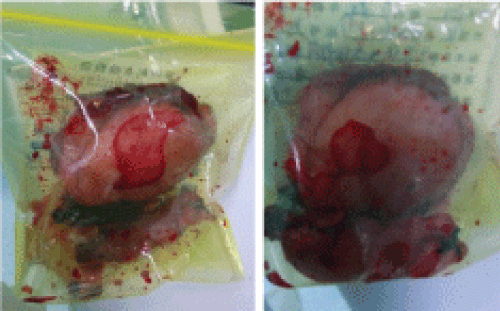
Figure 3: The excised rudimentary uterus including the right fallopian tube and ovary.
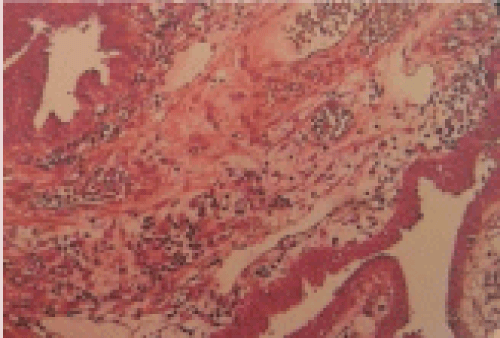
Figure 4: Histopathology image of the excised rudimentary uterus.
Discussion
Rudimentary uterine horn is a rare clinical condition resulting from congenital malformation of female genital tract during embryogenic development. This condition arises following an abnormal development of uterus cervix and upper vagina. Less than 400 cases has been reported in published literature till now [1] regarding this anomaly. During embryogenic period female reproductive organ develops at approximately 6 week of gestation from paired mullerian duct. This then descend medially within the mesenchyme and fuse with the opposite duct. A single cavity is then produced by the fused septum which then meets the upward growing urogenital sinus. A Result from failure of lateral fusion thought to give rise of Müllerian abnormalities including failure of vertical fusion or failure of resorption. For this case, the development of two separate rudimentary horns suggests failure of both lateral fusion and interruption of canalization. Unicornuate uterus is the failure of normal development of one of the paired mullerian duct [2]. Mullerian duct anomalies occur due to nondevelopment or abnormal development of the mullerian ducts or incomplete of resorption of the uterine septum [3]. “American Society of Reproductive Medicine” classified mullerian duct anomaly in to following:
A. Unicornuate uterus with communicating rudimentary horn.
B. Noncommunicating rudimentary horn with or with- out cavity.
C. An isolated unicornuate uterus [4].
A meta-analysis study by Nahum concluded that Uterine anomalies were identified in 1 in 594 fertile women (0.17%) and in 1 in 29 infertile women (3.5%) [5]. Though total reported incidence of unicornuate uterus is less than 400 in all scientific literature as reported by Yasmin Jayasinghe [1].
A symptomatic patient with rudimentary uterus may present with dysmenorrhoea, chronic pelvic pain, acute abdomen, hematometra, hematosalpinx and symptoms related with endometrosis [6,7]. In this case the patient is young 14 years old and presented with an acute lower abdominal tenderness and history of dysmenorrhoea. Initial ultrasonography was unable to provide a specific conclusion, so after a careful on patient’s condition a laparoscopic examination appeared as the most judging decision. This was done immediately and the diagnosis was confirmed as rudimentary uterine horn with a left sided ovarian cyst and surgical excision was performed. A case of rudimentary uterus is clinically misleading and the diagnosis is often difficult. Especially those cases presents with acute symptoms. A Laparoscopy is always a useful intervention for diagnosis of uterine anomaly aside of the radiological confirmation by hysterosalpingography, MRI and hysteroscopy. Beside that also Ultrasonography plays a vital role.
Conclusion
Rudimentary uterus is one of the rarest congenital malformations of uterus .We believe that our case presented here will provide additional point to the overview of rudimentary uterus and will be significant view for studies of congenital anomalies of uterus.
7092
References
- Jayasinghe Y, Rane A, Stalewski H, Grover S (2005) The presentation and early diagnosis of the rudimentary uterine horn.ObstetGynecol 105: 1456-1467.
- Robbins JB, Broadwell C, Chow LC, Parry JP, Sadowski EA (2015)Mullerian duct anomalies: embryological development, classification, and MRI assessment. Journal of magnetic resonance imaging: JMRI41:1-12.
- Khati NJ, Frazier AA, Brindle KA (2012)Theunicornuate uterus and its variants: clinical presentation, imaging findings, and associated complications. Journal of ultrasound in medicine: official journal of the American Institute of Ultrasound in Medicine31:319-331.
- [No authors listed] (1988) The American Fertility Society classifications of adnexal adhesions, distal tubal occlusion, tubal occlusion secondary to tubal ligation, tubal pregnancies, müllerian anomalies and intrauterine adhesions.FertilSteril 49: 944-955.
- Nahum GG (1998) Uterine anomalies. How common are they, and what is their distribution among subtypes?J Reprod Med 43: 877-887.
- Heinonen PK (1997) Unicornuate uterus and rudimentary horn.FertilSteril 68: 224-230.
- Liu MM (1994) Unicornuate uterus with rudimentary horn.Int J GynaecolObstet 44: 149-153.









