Research Article - (2022) Volume 0, Issue 0
Lack of Sleep and its Repercussion on Rotating Medical Interns at the Pablo Arturo Suarez General Hospital 2017 and 2018
Elias Celi1*,
Esteban Tafur Delgado2,
Aaron Alberto Guzman Tello3,
Jessica Nicole Ordonez Reyna4,
Maria Belen Vega Carvajal5,
Cristhian Enrique Sanipatin Mora6,
Luis Miguel Terán Cevallos7 and
Jorge Fabara8
1General Physician, Healing Clinic, Universidad de las Americas, Quito, Ecuador
2Third Year Resident of Pediatrics, Universidad del Sinú, Monteria, Colombia
3General Physician, Torre Medicina Clínicas Pichincha, Universidad de las Americas, Quito, Ecuador
4General Physician, Clinica Americana Adventista, Universidad de las Americas, Quito, Ecuador
5General Physician, Hospital Basico Clinica Jerusalen, Universidad de las Americas, Quito, Ecuador
6General Physician, Hospital Luis Gabriel DAvila, Universidad de las Americas, Quito, Ecuador
7General Physician, Healing Clinic, Universidad de las Americas, Quito, Ecuador
8General Physician, Nova Clinica Moderna, Universidad de las Americas, Quito, Ecuador
*Correspondence:
Elias Celi, General Physician, Healing Clinic, Universidad de las Americas, Quito,
Ecuador,
Email:
Received: 24-May-2022, Manuscript No. Iphsj-22-12798;
Editor assigned: 26-May-2022, Pre QC No. Iphsj-22-12798 (PQ);
Reviewed: 10-Jun-2022, QC No. QC No. Iphsj-22-12798;
Revised: 15-Jun-2022, Manuscript No. Iphsj-22-12798(R);
Published:
22-Jun-2022, DOI: 10.36648/1791-809X.16.S7.956
Abstract
Sleep, rest, is a complex physiological process, but that, however, is extremely important for our body to function properly, both in structural and functional terms, as well as in our interaction with the environment Introduction: In Ecuador, as surely in many hospitals in Latin America, especially public, the demands on rotating inmates are extremely great. These demands lead to sleep deprivation and therefore sleep rest. This deprivation generates alterations in the correct functioning of the organism and also entails behavioral alterations that are detrimental to the attention of patients.
Materials and Methods: A descriptive study was carried out, using as a tool a questionnaire of 6 closed questions. This questionnaire was distributed and carried out digitally by 76 rotating inmates of the Pablo Arturo Suárez General Hospital between 2017 and 2018.
Results: It was evidenced that 70% of the rotating medical inmates felt more tired between 00:00-03:00 am, 15% between 03:00-04:00 am, 6% between 06:00 am and 12:00 pm and finally 6% responded between 12:00-18:00 pm. No inmates reported feeling affected between 04:00-06:00 am. When it was inquired about how many hours are necessary to partially recover, it was evident that 42.9% required at least 3 hours of sleep, 42.9% 2 hours, 3.6% 1 hour, 3.6% 45 minutes and finally 7.1% 30 minutes. According to the survey, the services where a greater affection was evidenced by lack of sleep were Neonatology with 42%, Emergency in 27% and Surgery in 24% and Internal Medicine in 6%. When it was indicated which services generated a greater time of diversified occupation per service, it was evident that emergency and gynecology were the least monotonous with 25% and 21%, while the most monotonous were surgery 14% and neonatology 4% respectively. We also observed that theorization of mechanisms to reduce sleep during the guards were frequent, among them: Sweets: 27%, Music: 24%, Coffee: 24%, Drinks and stimulants other than coffee: 18%, medicine 3%, nothing: 3%; 48% answered that the various methods used partially help, 38.7% mentioned that they do not help and 12% answered that they do help
Conclusions: Lack of sleep and with it the lack of rest in rotating inmates affects their health, but also their action and behavior with patients. It is important to reduce the working day, improve the treatment of rotating inmates, diversify their tasks and perhaps, facilitate activities or resources that improve their status and performance.
Keywords
Lack of sleep; Impact; Internal doctors; Rotation
Introduction
There is no doubt that scenarios such as intensive care, emergency,
pediatrics, among others, are places where the dynamics,
articulation and development of the operating personnel of the Pablo Arturo Suárez General Hospital is highly mobile, but above
all, highly concentrated, so that the response that doctors, nurses,
assistants, interns must give must be timely, scientific and, of
course, affable; To this extent, these interventions, either due to
the numerical product of the demand and its quality, require that
the inmates and other medical personnel be in optimal physical,
psychological and cognitive conditions.
The long periods of work without rest and without sleep, finally
end up undermining the cognitive capacity of individuals, reducing
the ability to function at an acceptable level and is incompatible
with the expectation of the hospital patient. Under this premise,
it is important to develop procedures that allow inmates and
their leaders to obtain, in normal periods, the amount of rest
and minimum sleep necessary to ensure that the response is
concurrent to each of the scenarios to be confronted.
The difficulties that the state has to provide infrastructural
responses and hospital services at the different levels of care,
has determined that the existing ones assume and absorb the
demand of users that apparently grow exponentially.
Precisely the Pablo Arturo Suárez General Hospital, after an
important remodeling process in 2015, it is understood that
it should serve approximately 300,000 users annually, “with
an average of 850 people a day; 650 in the 33 specialties in 75
offices and 18 subspecialties, and 200 through emergency, since
it increased from 20 to 60 attention posts” [1].
However, as of 2017, in this hospital, 149,111 patients were
treated in the outpatient area, 85,379 in emergency; and, in part
of 2018, in external consultation 98,861; 43,663 in emergency
(August 2018) and 7,337 graduates. Definitely, public hospitals
have become scenarios where the greatest contradictions of the
entire public apparatus converge, in which affirmative action,
timely, effective care, has a bloody struggle with the limitations
of not having enough operating personnel, supplies physicians,
and a high volume from users.
The new hospital system has been redirected on its true
objectives. It aims to provide greater care coverage, but this, to
some extent, ignores quality by improving numerical indicators.
Quantity for quality and the results can often be disastrous. In
philosophical terms, the quantitative vision of any phenomenon,
whether natural or social, and in this case, an eminently social
phenomenon is biased, unilateral and even mechanistic; On the
other hand, a purely qualitative view of the same phenomenon
can have the same bias, and even become exclusive. Not
understanding that the leaps in quality are necessarily linked
to those in quality will keep us tied to constantly replicating the
error that does not match the requirements of our people. It
must be recognized that political clientelism also interacts behind
this quantitative phenomenon, opening up public services on
the same infrastructural base, generating hospital congestion
and with it, weakness in the quality of care. The institutional
response is not isolated; it is supported by certain state policies.
For example, setting care quotas, a number of patients seen
by a doctor on a given day; or, the other, the incorporation of
nursing and medical students to public hospitals under the figure
of pre-professional practices to support a system that is weak, anemic. Pre-professional practices, community practice and
later rural, would seem to be a euphemism for labor exploitation
that contains a series of contradictions that the state cannot
solve. Although it is true that it is fundamental in the process of
training a doctor to carry out their pre-professional practices in
real conditions, limited to the strengths and weaknesses of the
health system offered by the state, the design of how to do it and
under what conditions should change., and in a dramatic way,
so that this process is instructive, formative, that strengthens
the student, but not that it weakens him in his vocation or the
methodological process of approaching the patient.
And of course, this is not just a problem for students, but also for
a certain level of doctors, nurses, administrative staff and others,
who are subjected to high workloads, with exhausting guards,
which in many cases humanly cannot be dealt with efficiently.
In the case of the students who carry out the rotating internship
at the Pablo Arturo Suárez General Hospital, which is practically
identical to what happens in the other hospitals and public care
centers in the country-, they are subjected to long hours of work,
especially all those that compromise the guards whose days go
from 24 to 28 hours (not infrequently they extend a couple of
hours more) of service in which they put in tension the knowledge
acquired in the classroom, in addition, they incorporate their own
knowledge of the daily life of a hospital, whether in objective
aspects such as the scientific treatment of patients, clinical and
medical procedures; as well as in subjective aspects that go from
the interaction with administrative and operational personnel
of the Hospital, the same that is not necessarily affable, cordial,
on the contrary, they exercise a behavioral, vertical relationship,
which often acquires aggressive, imperative and deeply
subjective characteristics., which regularly, instead of forming,
deform the future doctor's personality. As Machado would say,
"with the thread they give us, we weave, when we weave" helps
to better describe what happens with the interns and their stay in
their practices (internship) at the Hospital General Pablo Arturo
Suárez, and perhaps, the thread that rotating interns have in
their hands is precisely the limitations in means added to the high
workload that is evident, qualitatively and quantitatively, in the
care they give to patients [2].
Materials and Methods
A descriptive study was carried out, using as a tool a questionnaire
elaborated through "Google Forms", which consisted of 6 closed
questions. Said questionnaire was distributed through an instant
messaging service "Whatsapp", which was carried out digitally by
76 rotating interns of the Pablo Arturo Suárez General Hospital
between 2017 and 2018.
Results
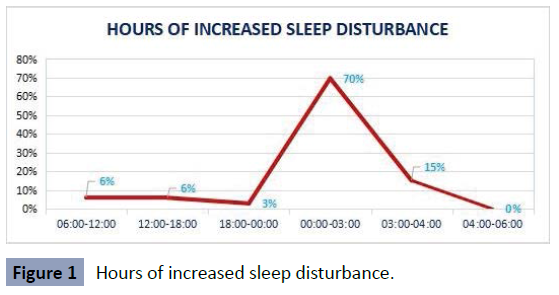
It was found that 70% of the rotating medicine interns felt more
tired between midnight and three in the morning, followed by
15% who felt more tired between three and four in the morning,
approximately. 6% between six in the morning and twelve in the
afternoon and another 6% between twelve in the afternoon and
six at night. No rotating intern felt particularly affected between
4 and 6 in the morning (Figure 1).
Figure 1: Hours of increased sleep disturbance.
Now, the issue is how much sleep is required to be able to recover
in an elementally operational way? In one of the questions that
were asked to the rotating medical interns of the Pablo Arturo
Suárez General Hospital, they state that the minimum rest should
be between 2-3 hours, with 3 hours of sleep being prevalent;
that, with that time, efforts can be renewed to sustain the long
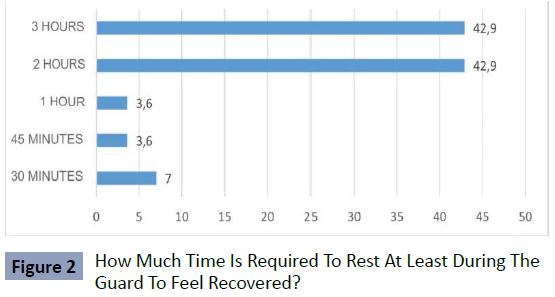
journey. As we observed, 42.9% mentioned requiring at least 3
hours of sleep to feel rested, 42.9% referred requiring at least 2
hours, 3.6% 1 hour, 3.6% 45 minutes and only 7.1% mentioned
30 minutes as the time needed to feel moderately recovered
(Figure 2).
Figure 2: How Much Time Is Required To Rest At Least During The
Guard To Feel Recovered?.
When the students are asked in which service they feel more
affected by the lack of rest, they all agree that in those where
the activities are monotonous, repetitive that, however, in
those services where there is more activity, more movement,
but more diversity of activities, sleep can be better managed.
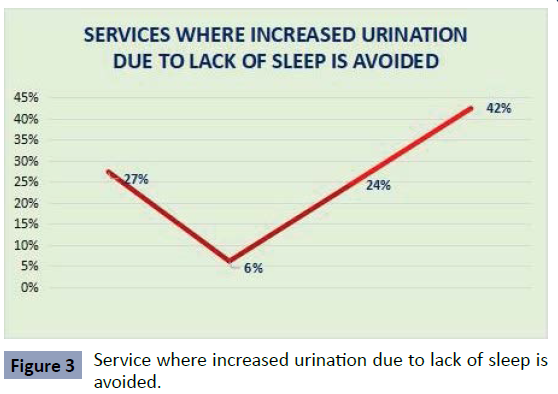
As we observed in the results of our survey, the services where
the greatest affectation was evidenced by lack of sleep were
neonatology with 42%, followed by emergency with 27%, surgery
with 24% and finally internal medicine with 6% (Figure 3).
Figure 3: Service where increased urination due to lack of sleep is
avoided.
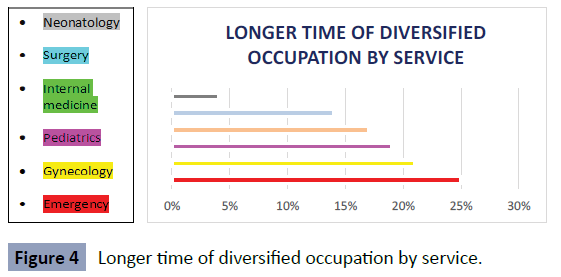
On the other hand, the longest occupancy time diversified by
service and that had the least impact due to sleep deprivation
were emergency with 25%, gynecology 21%, pediatrics 19%,
internal medicine: 17% while the most monotonous were surgery
14% and neonatology 4% (Figure 4).
Figure 4: Longer time of diversified occupation by service.
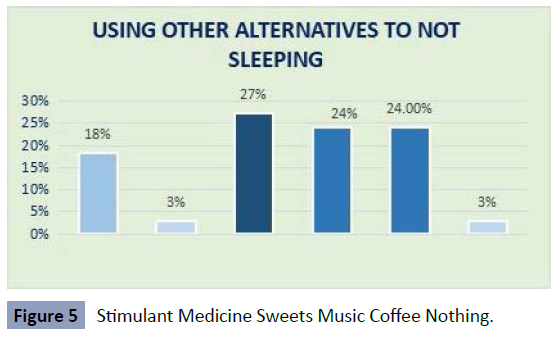
On the other hand, it was intended to investigate what
mechanisms the rotating medicine interns used to reduce
sleep and therefore fatigue while they were active in each of
the services. It was observed, within the hospital population,
especially among rotating interns, the consumption of sweets,
chocolates and the like are the most used, music is another
element that helps to stay active despite fatigue and, obviously,
the use of stimulating drinks other than coffee, such as 220V, Red
Bull and others. As we can see, the rotating medicine interns at
Pablo Arturo Suárez General Hospital mention the use of sweets
by 27%, music by 24%, coffee by 24%, stimulating drinks other
than coffee by 18%, medicine by 3% and nothing at 3% (Figure 5).
Figure 5: Stimulant Medicine Sweets Music Coffee Nothing.
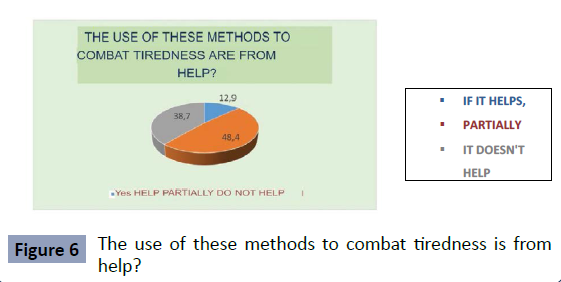
However, the consumption of these substances or the use
of music to try to stay awake is not necessarily presented as
definitive solutions. As we evidenced, 48% responded that the
various methods used help partially, 38.7% mentioned that they
do not help and 12% answered that they do help (Figure 6).
Figure 6: The use of these methods to combat tiredness is from
help?.
Discussion
It is very important to mention that, like all factors in the
human body, sleep is closely related to the general state of
physical, emotional and psychological health [3, 4] The amount
of hours that should be dedicated to sleep will depend on the
organism, the environment and the behavior, since this can have
considerable variations in each person. So we can talk about 3
sleep cycles, short, intermediate and long sleep cycle [5]. In this
way, we speak of efficient and good quality dream cycles. An
alteration in a person's sleep cycle can greatly affect their health
and psychological state, making them more prone to making
mistakes at work and generating high stress loads [6].
One of the professions most affected by lack of sleep and which
are exposed to long working hours are the medical professions,
especially when they complete their year of internship at the end
of their academic period, which causes many of these professions
to suffer from burnout syndrome, this is characterized by
symptoms such as fatigue, irritability, both mental and physical
exhaustion, which generates consequences such as medical
errors, misdiagnosis, wrong procedures, among others, where
the safety of both the patient and the patient would be exposed.
Of the same professional [7, 8] Due to extreme fatigue, skills such
as critical analysis and correct decision making are lost, which
would directly affect patients [9].
In a study carried out by the researcher Karen Cecilia Chacaltana
Linares et al, worrying figures were obtained on the frequency
with which burnout syndrome occurred in interns during their
year of internship in several hospitals in Lima, where they
participated in the study 165 medical interns: 52% (85 people) of
the internship, from the year 2017; and 48% (80 people) of the
boarding school, from the year 2018. The participants were on
average between 22 and 25 years old, female and male, single
and without children. It was found that 81.3% of the interns of
the year 2018 described their sleep cycle from "fair to very bad",
while more than half of the interns of the year 2017 described
their sleep cycle "very good and good" in a 55.3%. The frequency
of burnout syndrome in medical interns was 33% and 35%, for the
year 2017 and 2018, respectively. All this related to the increase
in the working day and a decrease in recreational activities by
intern doctors [10].
Cognitive skills are essential for all the daily activities carried out
by interns, multiple studies confirm that doctors and personnel
in the health area are vulnerable to problems related to cognitive deterioration, this generated by long hours in those who stay
awake, extended and repetitive 24-hour shifts. Factors such as
tiredness and lack of sleep can develop major problems, such as
high levels of stress, depression, obesity, cardiovascular diseases,
hypertension, psychological disorders, among other pathologies.
The most likely to suffer from these conditions are the young
population between 22 at 30 years of age, in addition to that,
their basic skills, concentration, and techniques that are used at
the time of patient care decrease, they also slow down, when
responding to an emergency [11]. Due to the fact that internal
doctors play a double role during their internship year, since they
provide hospital care and at the same time they are finishing their
academic training process, it generates greater pressure and quite
high stress levels. Likewise, as affirmed by Dr. Sánchez-Amo L et
al., in his study on the influence of stress and long working hours,
which are related to high levels of incidence of errors committed
during patient care. In his research, he affirms that excessive
hours and work overload generate emotional stress and fatigue,
which affects the performance of doctors and the management
of patients. In this study, an investigation was carried out in the
existing medical bibliography, where a data collection was made
in order to generate improvement in the quality of patient care.
Several studies conducted in New Zealand, the United States,
Canada, among others, were found, where a large percentage
of professionals acknowledged being exposed to long working
hours, which greatly alters their sleep cycle, especially doctors in
training where Due to the high levels of fatigue, their incidence
of error was 36% and self-injury with sharp objects was 61% [12].
Conclusions
It is evident that the incidence of lack of sleep in the rotating
interns of the Pablo Arturo Suárez General Hospital is important.
That this incidence varies depending on the service, despite
the shifts or occupational time being the same. The greater
the monotony, the greater the affection, the greater the
diversification of activities, the conditions change notably. For
the purpose of this study, there is full agreement with the studies
cited and that are related to the fact that the time of greatest
physical, psychological and cognitive depression due to lack of
sleep is at 03:00 am, a space in which it is important to consider
countermeasures, one of them being the use of micro-sleep to
be able to recover the inmate in relatively acceptable operating
conditions. It is conclusive the fact that the management of the
fatigue of the rotating interns of the Pablo Arturo Suárez General
Hospital depends a lot on the capacities, creativity and good
judgment of the leaders. The correct dosage of time, tasks and
how to carry out the different activities will pay the students
so that they can better manage their fatigue, sleep, and the
predisposition to be able to fulfill the assigned tasks.
In any case, it could be concluded that:
• The academic/operational performance of rotating
interns is lower in individuals who have greater difficulties in
managing sleep deprivation.
• That the greatest condition resulting from lack of sleep
is physical, however, the most dangerous in operational terms is
the loss of cognitive abilities.
• That the use of stimulant beverages other than coffee
may eventually help to manage the lack of rest/sleep, however
the subsequent consequences may be detrimental to the
apparent benefit they provide.
• That the correct leadership of those responsible
(heads) of the floor or service, can achieve, with appropriate
countermeasures, that the rotating interns and other hospital
personnel dose their rest in such a way that their responses to the
requirements of the hospital and of the patients Be as objective
and optimal as possible.
• That generating affable, friendly interpersonal
relationship spaces help to better manage the stages of
exhaustion.
REFERENCES
- Ciudadano E, El ciudadano (2015) Obtenido de 300 mil pacientes al ano puede atender el nuevo Pablo Arturo Suarez.
Indexed at, Google Scholar
- Machado A (2004) Select Poems of Antonio Machado. En W. Barn stone. New York: Copper Canyon Press Obtenido de.
Google Scholar
- Morales J, Yanez A, Fernandez-Gonzalez L, Montesinos-Magraner L, Marco-Ahullo A et al. (2019) Stress and autonomic response to sleep deprivation in medical residents: A comparative cross-sectional study 14:e0214858.
Indexed at, Google Scholar, Crossref
- Schwartz L P, Hursh S R, Boyle L, Davis J E, Smith M et al. (2021) Fatigue in surgical residents an analysis of duty-hours and the effect of hypothetical naps on predicted performance. Am J Surg 221:866-871.
Indexed at, Google Scholar, Crossref
- Vilchez-Cornejo J, Viera-Moron R D, Larico-Calla G, Alvarez-Cutipa D C, Sanchez-Vicente J C et al. (2020) Depression and abuse during medical internships in Peruvian hospitals, Duty Hour Regulations of Physicians in Training and Circadian Considerations. Circadian Rhythm Sleep-Wake Disorders ombiana de Psiquiatría. Revista Col Olson E J 49:75-82.
Indexed at, Google Scholar, Crossref
- Fowler L A, Ellis S (2019) the effect of 12 hour shifts, time of day, and sleepiness on emotional empathy and burnout in medical students. Clocks Sleep 1:501-509.
Indexed at, Google Scholar, Crossref
- Carrasco J P, Ferrando M, Jimenez M, Martin J, Martínez E (2021) Se sobrecarga a los médicos residentes? Estudio descriptivo sobre la falta de libranza de guardias de los médicos residentes y análisis de sus consecuencias docentes en la provincia de Valencia. Educación Medica 22:98-105.
Indexed at, Google Scholar, Crossref
- Arteaga Gende M R (2021) Deterioro cognitivo en médicos residentes por la privación Del sueño en guardias de 24 horas. Revista San Gregorio 1:174-191.
Google Scholar, Crossref
- Vallejo-Noguera FF, Rubio-Endara O W, Medranda-Zambrano RG (2019) Riesgos psicosociales en personal médico que labora en el Hospital Rodríguez Zambrano en Manta, Ecuador. Dominio de las Ciencias 5:4-18.
Indexed at, Google Scholar
- Linaresa K C C, Cama L F R (2020) Persistencia del síndrome burnout en internos de medicina en hospitals de Lima Peru Investigation en educacion medica 8:9-15.
Indexed at, Google Scholar
- Gilces D C V, Nieves R R R, Abarca F L P, Velez L S I, Prado M M C (2009) Identificación y evaluation de los factores de riesgo psico-social en personal que labora en una central de llamadas de emergencia. Ecuador-2018. Archivos Venezolanos de Farmacología y Terapéutica 38:39.
Google Scholar
- Sanchez-Amo L, Sanchez-Rubiales M (2018) Influencia del estrés y la duración de la jornada laboral sobre el error medico. ACTUALIDAD M É DICA 148.
Google Scholar, Crossref
Citation: Celi E, Delgado JET, Tello AAG,
Reyna JNO, Carvajal MBV, et al. (2022) Lack
of Sleep and its Repercussion on Rotating
Medical Interns at the Pablo Arturo Suarez
General Hospital 2017 and 2018. Health Sci J.
Vol. 16 No. S7: 956.